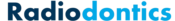Apical Radiopacities
Dr. Barett Andreasen, Oral and Maxillofacial Radiologist
This article serves as a review for the various radiopacities that are associated with the apices of mandibular and maxillary teeth. While this is by no means a complete and comprehensive list, these are the more common entities that will be encountered in the practice of dentistry.
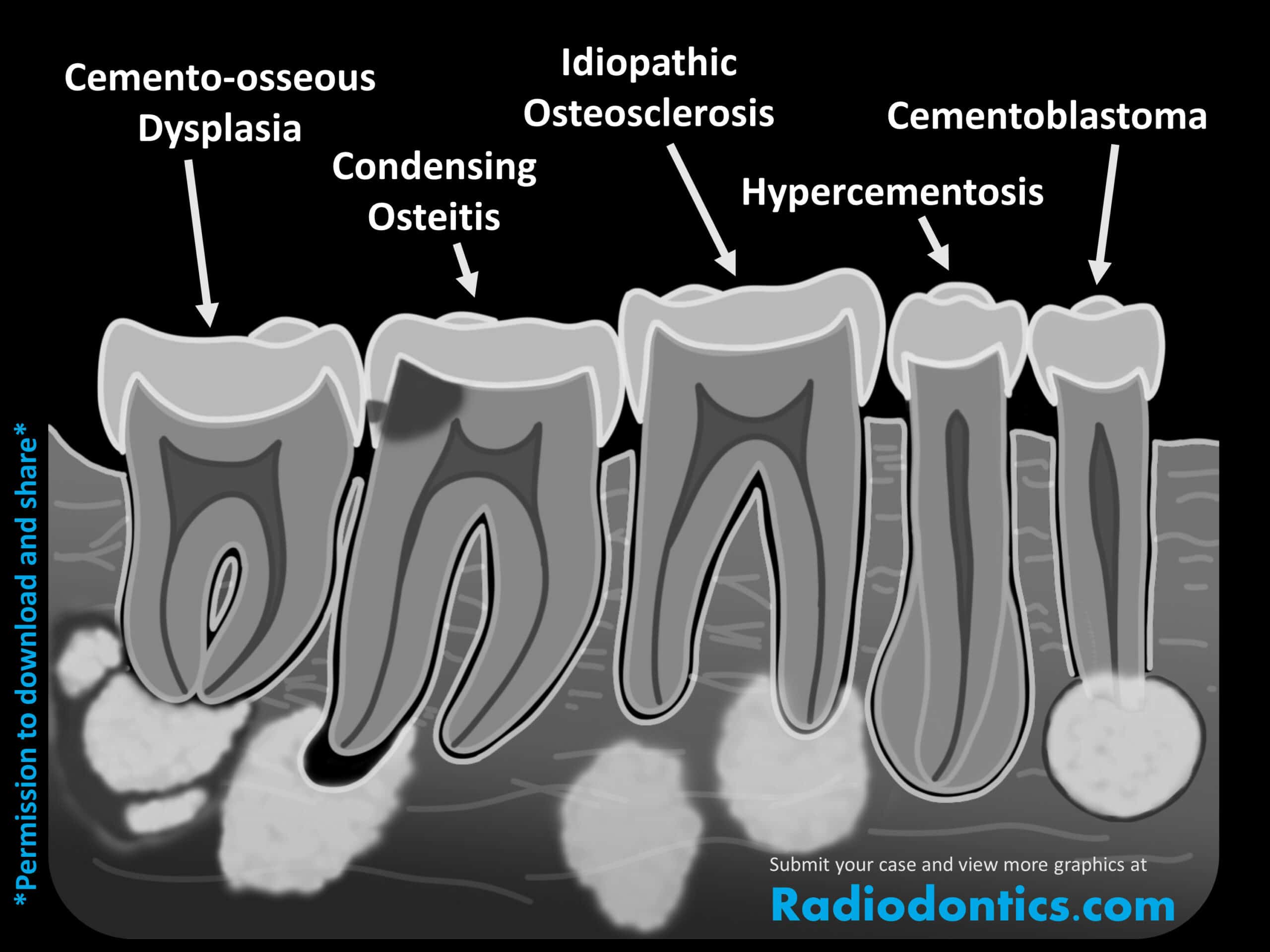
Cemento-osseous dysplasia
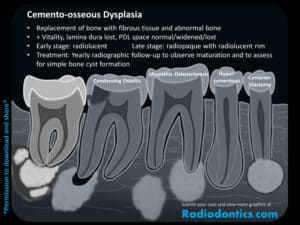
Cemento-osseous dysplasia is a replacement of the normal trabecular bone with fibrous tissue and cementum-like/abnormal bone. It begins as a well-defined radiolucency associated with the apices of teeth and as the lesion matures, radiopacities (often crescent-shaped) begin to appear around the tooth apex. Late stage lesions present as dense radiopacities with a radiolucent border surrounding it. There is often a periphery of sclerotic bone of varying width that may appear as a cortical outline. When cemento-osseous dysplasia directly involves the teeth, the lamina dura may be lost and the PDL space will either appear normal, widened or may be lost as well; however, the involved teeth remain vital, so please don't confuse an early lesion for periapical inflammation! If the lesion is large enough to involve the adjacent cortices, thinning and expansion of the cortices may occur.
There are three different variants of cemento-osseous dysplasia: focal, periapical, and florid. Focal cemento-osseous dysplasia involves a single site, typically in the posterior mandible. Periapical cemento-osseous dysplasia predominately affects the periapical region of the anterior mandible. Extensive forms of cemento-osseous dysplasia affecting 3 or more quadrants or widespread involvement in one jaw is termed florid cemento-osseous dysplasia.
An important fact in diagnosing cemento-osseous dysplasia is that it has a marked predilection for middle-aged to older black or Asian females.
No biopsy or treatment is indicated. However, regular radiographic follow-up (approximately every 12 months) is recommended to assess maturation of the lesion(s) and to monitor for simple bone cyst formation and secondary infection.
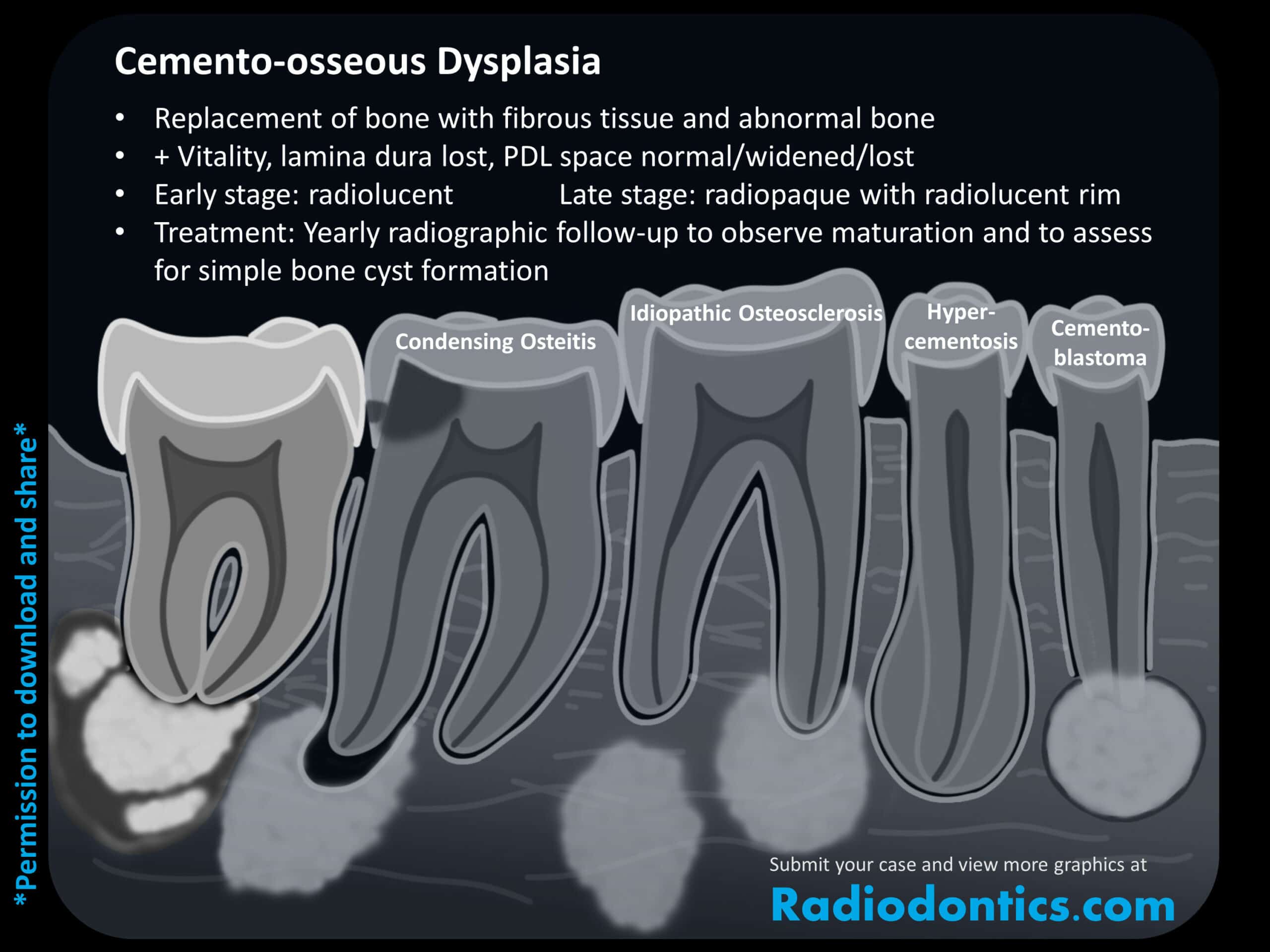
Condensing osteitis
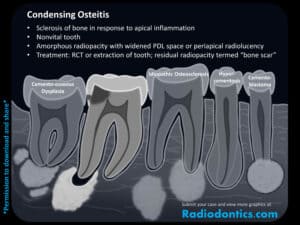
As the name suggests, condensing osteitis is a bony proliferation in response to inflammation and will therefore only be found at the apex of non-vital teeth (-itis = inflammation). This process appears as an irregularly-shaped sclerosis with a widened PDL space or periapical radiolucency between the root and the area of sclerosis. The sclerotic bone may remain after treatment of the inflammation and is termed as osteosclerosis or a bone scar. The key take away is that condensing osteitis is only associated with pulpal inflammation, while the other entities which may appear similar (idiopathic osteosclerosis, cemento-osseous dysplasia, hypercementosis, and cementoblastoma) are associated with vital teeth.
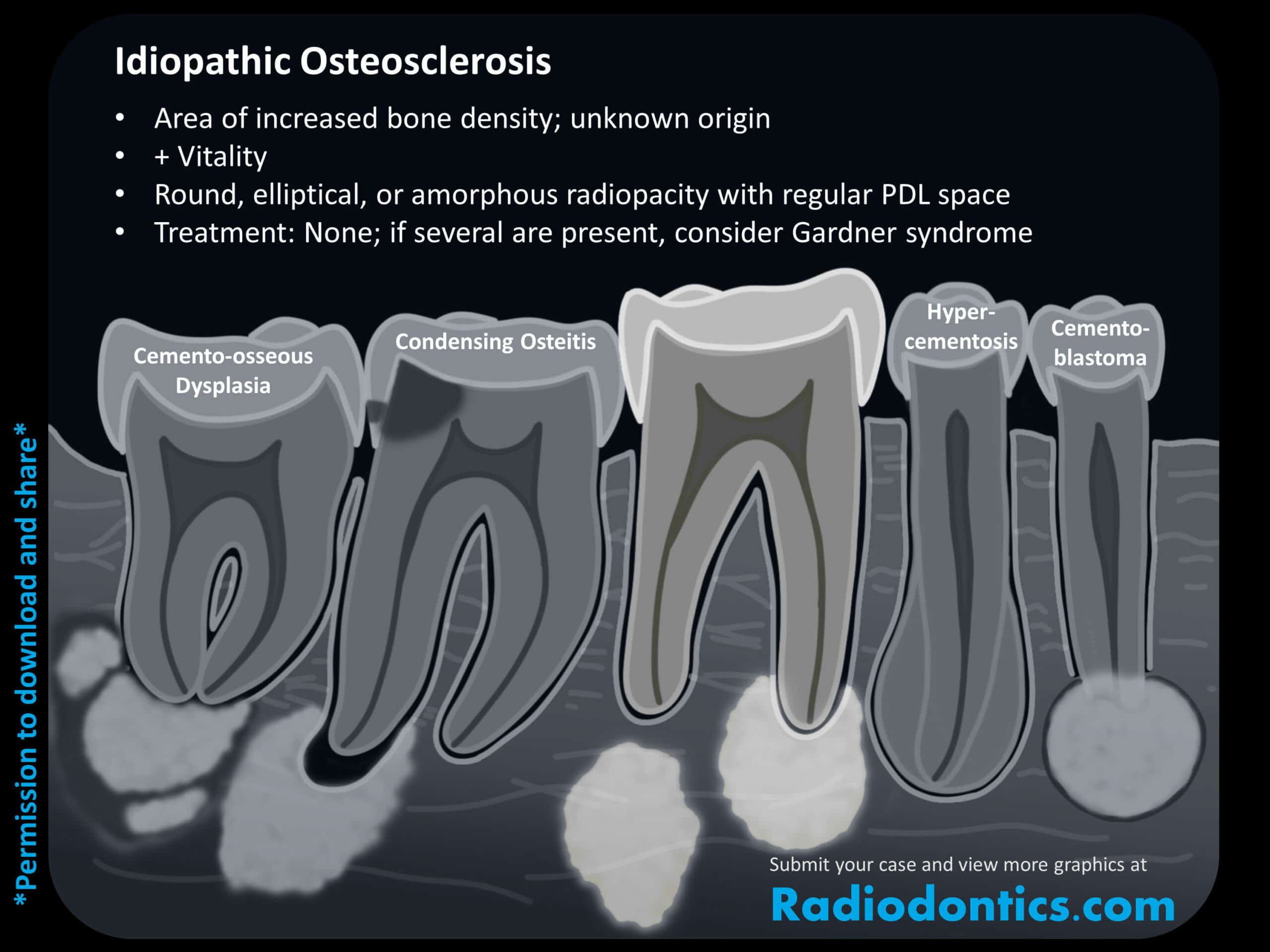
Idiopathic osteosclerosis
Also known as a dense bony island, enostosis, or hyperostosis, this finding is of unknown etiology and typically occurs in the posterior mandible. While often associated with the root apices of mandibular molars and premolars, it can be found anywhere within the jaws. Idiopathic osteosclerosis presents as a dense, homogenous radiopacity with an amorphous shape. When associated with a root, a regular PDL space is maintained and the tooth is vital. On a CBCT, it will blend into adjacent cortices with no thinning or expansion. These features help differentiate idiopathic osteosclerosis from similar entities such as condensing osteitis, cemento-osseous dysplasia, hypercementosis, and cementoblastoma. No treatment is necessary for areas of idiopathic osteosclerosis.
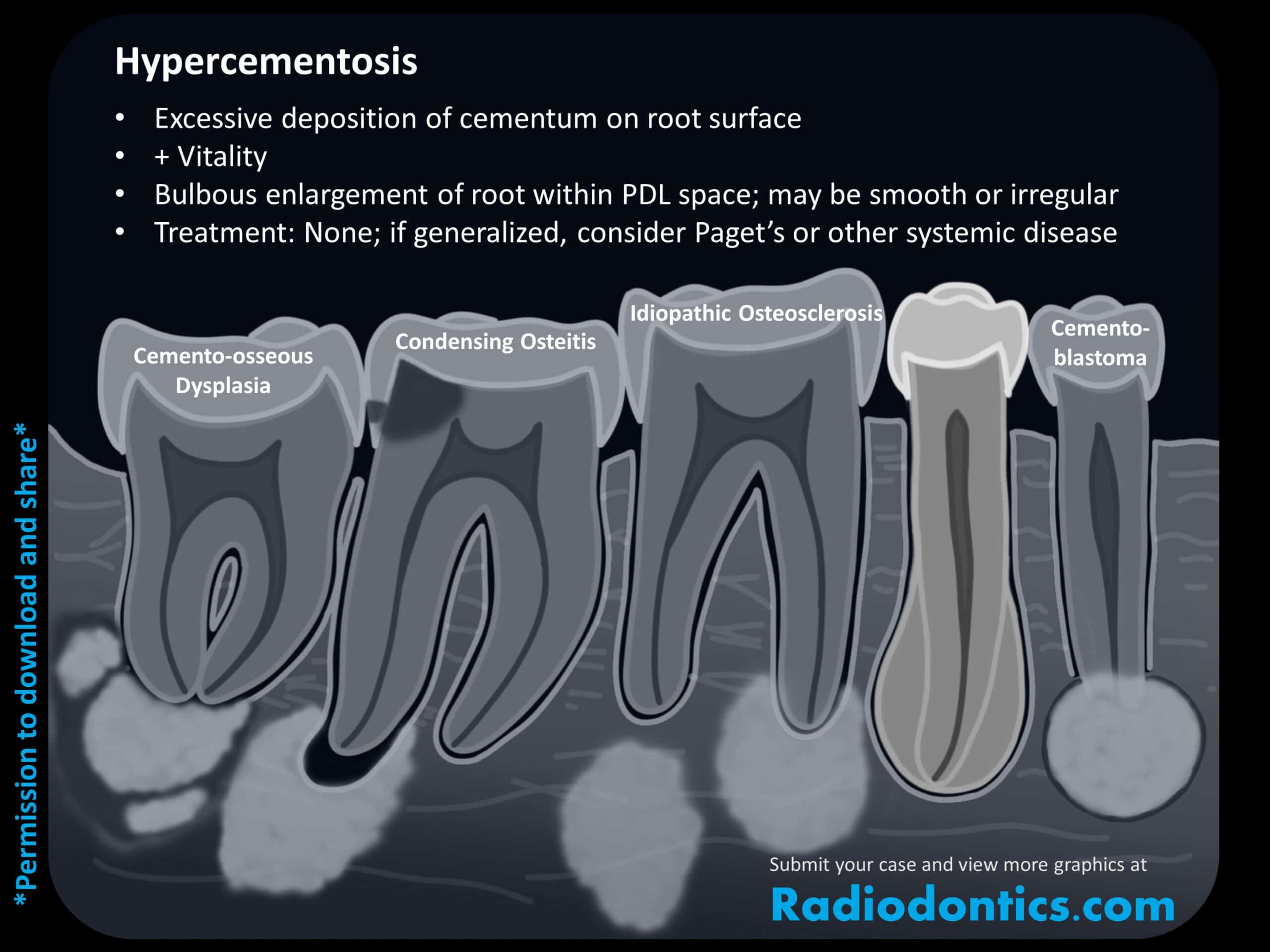
Hypercementosis
Hypercementosis, as the name implies, is the buildup of excess cementum on the root surfaces. This deposition of cementum typically occurs within the apical third on posterior mandibular teeth and may give the root a 'bulbous' appearance. Though the appearance is unusual, the tooth is vital and the PDL space and lamina dura will remain regular and continuous around the areas of hypercementosis. The exact etiology is unknown; however, it's theorized to be a response to unstable or changing occlusion. Conditions such as Paget's disease, hyperpituitarism and Gardner syndrome should be ruled out if the hypercementosis is generalized. No treatment is necessary; however, extractions of teeth with hypercementosis may prove to be more difficult due to the bulbous shape of the roots.
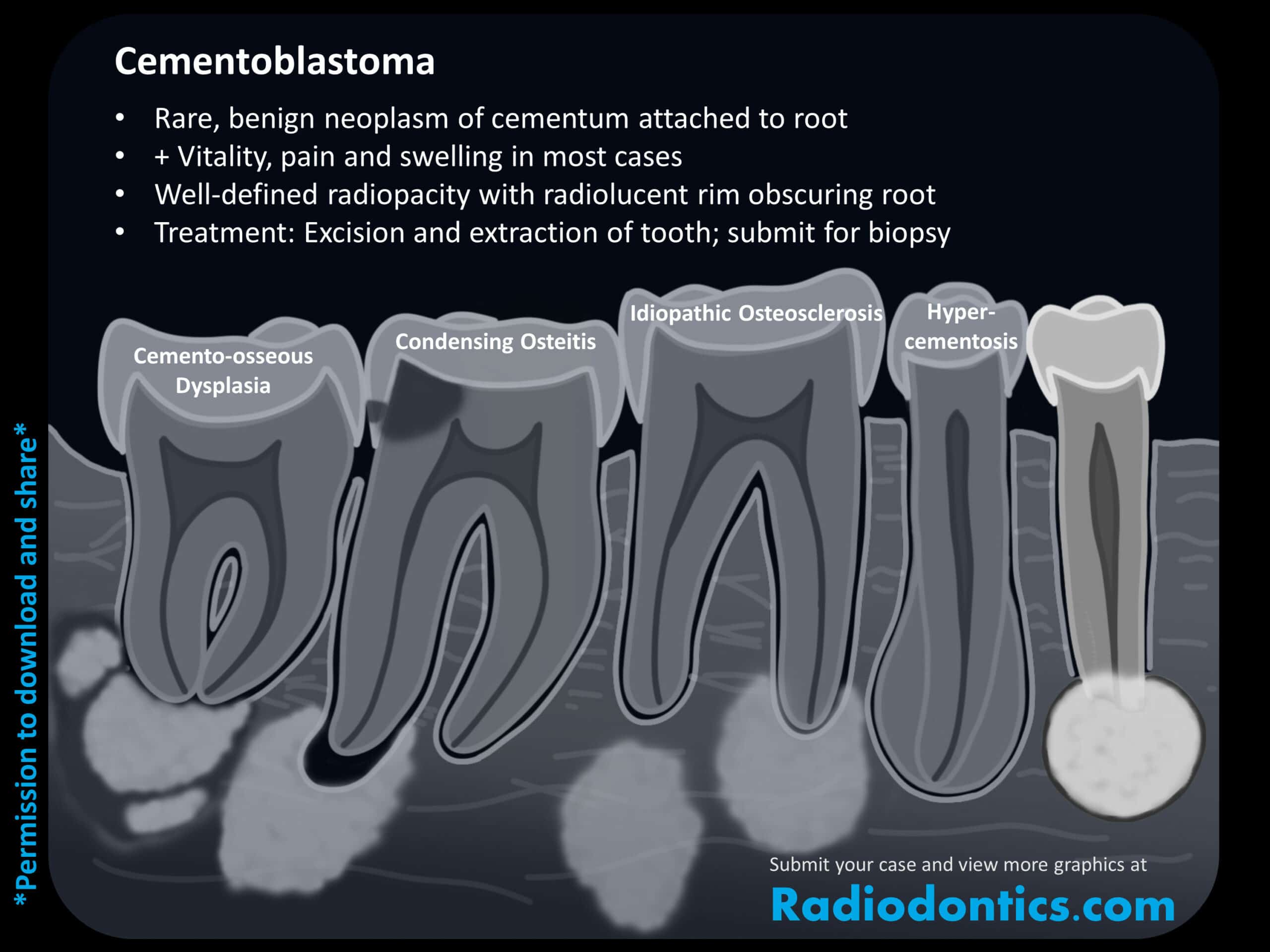
Cementoblastoma
A cementoblastoma is a benign odontogenic neoplasm of cementoblasts and cementum and is seen most frequently involving the mandibular premolars or first molars of young adults. Cementoblastomas appear as a well-defined radiopacity or mixed density lesion with an amorphous or spoke-wheel pattern attached to and surrounding the root of a vital tooth. The outline of the roots are usually obscured and external root resorption may be seen as well. Pain and swelling can also be present. Suspected cementoblastomas should be biopsied and sent for pathological evaluation.
A Few Tips
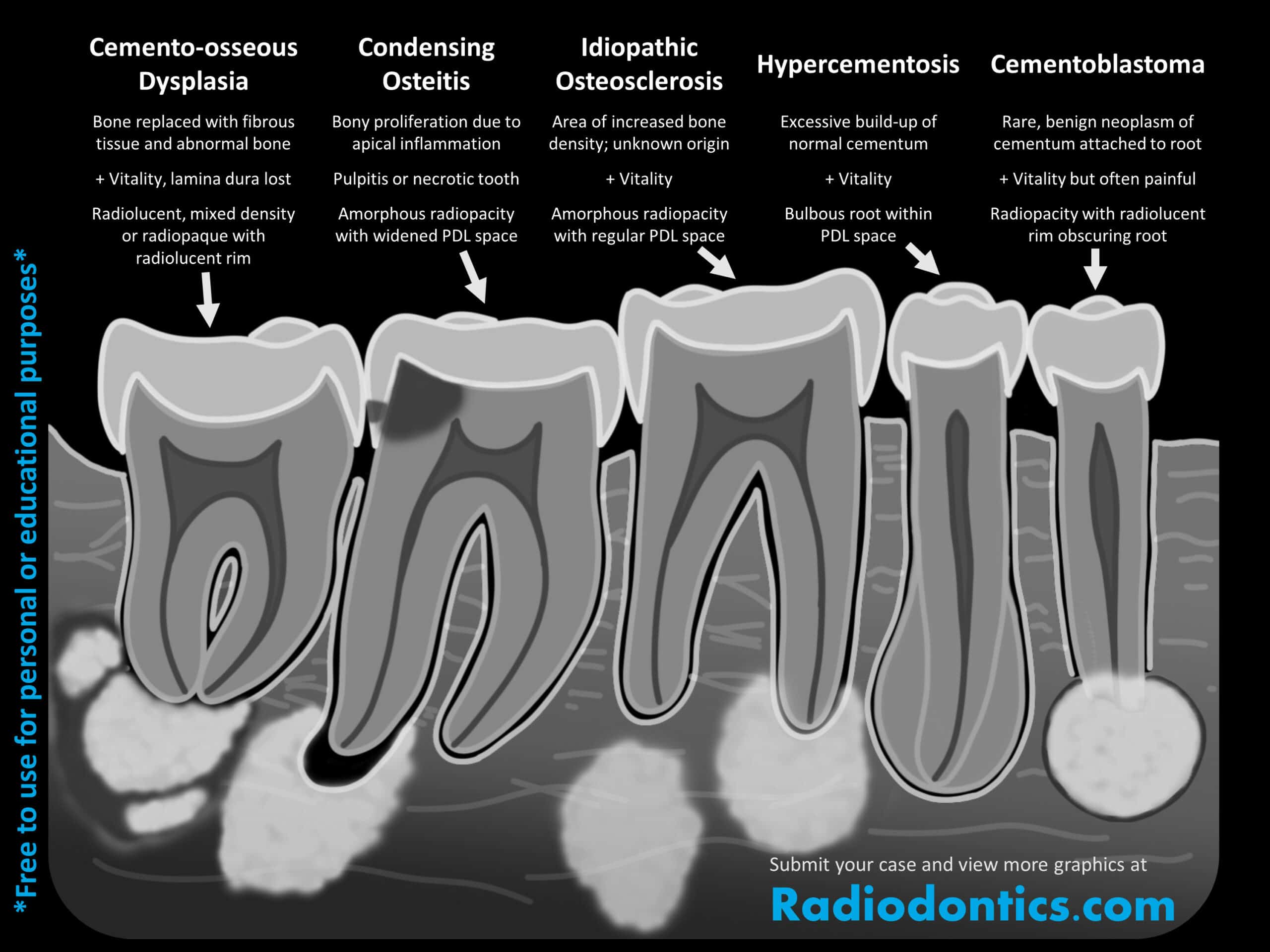
The most reliable way to distinguish between these several entities is to look at the relationship between the lesion and the lamina dura, the PDL space, and the root. Each lesion :
- Cemento-osseous dysplasia often causes loss of the lamina dura and the PDL may be normal, widened, or lost as well.
- Condensing osteitis is associated with PDL space widening or a periapical radiolucency.
- Idiopathic osteosclerosis will maintain a normal PDL space.
- Hypercementosis is contained within the lamina dura and PDL space, which are normal.
- Cementoblastomas are attached directly to the root and often obscures the root itself.
Vitality testing can also be performed on teeth with apical radiopacities to assist in diagnosis. All the entities above are associated with vital teeth with the exception of condensing osteitis. It's an easy one to cross off the list once you confirm tooth vitality.
A Word of Caution
There are, as always, exceptions to these rules. As anyone who practices in the field of dentistry knows, nothing ever quite follows the textbooks, especially when delving into the field of pathology and radiology. The entities covered above demonstrate many various presentations and manifestations which cannot be covered in this article, and that's not to mention the numerous pathologies which were not discussed.
If you have any questions about a radiograph, please click on the 'Upload Case' button below to have your images be reviewed by an oral and maxillofacial radiologist.